Sports Foot Injuries
Overview
Athletic competition provides numerous physical, mental, and social health benefits. But they often require the body to push much harder than it would otherwise.
Over time, such stress could cause injuries to various body parts. One such susceptible area is your feet, which can affect your ability to walk, move, and perform many other activities.
Athletes stand at an increased risk of developing any one of several sports foot injuries or even possibly a torn ligament. Read on to learn about specific sports-related foot injuries and possible treatments.
PLANTAR FASCIITIS
Anatomy
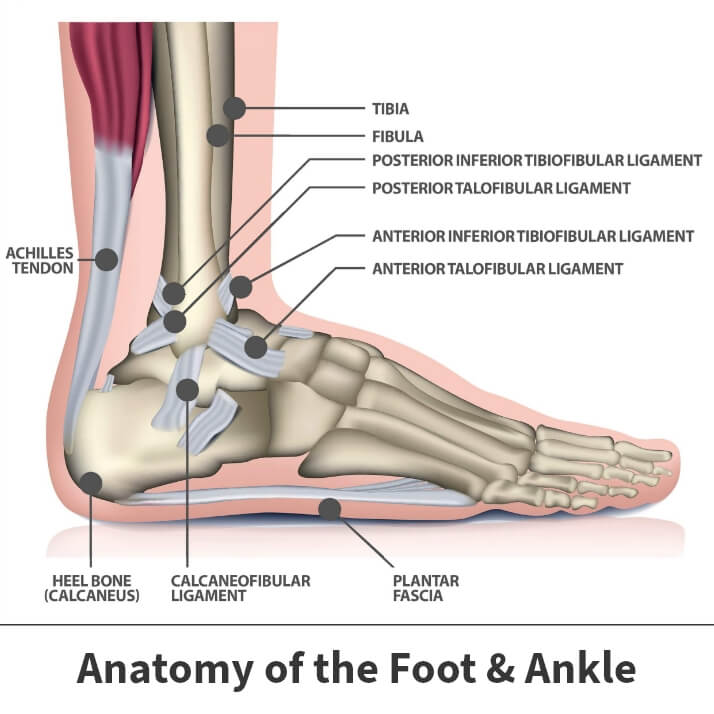
Situated near your foot’s arch is a collection of tissue known as the plantar fascia.
Description
When plantar fascia encounter excessive stress and strain, they can grow irritated and inflamed. This condition is referred to as plantar fasciitis.
Causes
Plantar fasciitis can be brought on by athletic activities that place significant stress on your arches, such as running, soccer, and basketball.
Symptoms
The most obvious symptom is pain near your heel. This discomfort can vary in intensity and might worsen when you step down or engage in any activity that places stress on the arches. Other symptoms include redness and swelling around the heel or foot’s bottom.
Diagnosis
Typically, diagnosis is not difficult. Pain in the arches and inflammation during examination often confirm the condition. Your doctor may order diagnostic imaging tests to rule out other conditions.
Treatment Overview
Only severe cases will require surgery. Most incidents respond favorably to less invasive treatments.
Non-Surgical Treatment Options
Minor instances might respond to over-the-counter medications like pain reducers and non-steroidal anti-inflammatory agents, which are commonly abbreviated as NSAIDs. This includes Advil or Motrin (ibuprofen) and Aleve or Naprosyn (naproxen).
More moderate cases might call for the use of night splints, which keep your foot’s arch stable while you sleep. Other options could include a course of physical therapy or the insertion of padded inserts (orthotics) into your shoes to provide added protection and cushioning.
Other more significant non-surgical therapies might include electric therapy (in which impulses are transmitted into the plantar fascia) and steroid injections.
Surgical Procedures
Two types of surgery are typically performed in the most severe instances of plantar fasciitis.
The first is ultrasound, where waves break up and eliminate ailing tissue. As a last resort, a surgeon might need to remove the plantar fascia from the heel bone.
STRESS FRACTURES
Anatomy
The feet and ankles are comprised of many bones. Many of these bones weaken when exposed to the stress placed on them during repeated athletic competition.
Description
Stress fractures occur when any of these bones incur tiny breakages. In medical terms, these events are called stress fractures.
Causes
Stress fractures are often the result of a quick, damaging event like a fall or collision or having your foot stepped on. Gradual bone weakening can also lead to the problem.
Symptoms
The clearest indication you might have a stress fracture is moderate to severe foot or ankle pain. However, in many instances, such discomfort:
- Increases when putting weight on the foot.
- Lessens when you are at rest.
- Intensifies when running or jumping.
- Appears when the area is touched or pushed into.
You might also experience symptoms like inflammation near the damaged bone or outward signs of bruising.
Diagnosis
Physicians often cannot confirm a stress fracture’s presence without the use of diagnostic imaging tools such as X-rays, magnetic resonance imaging (MRI scans) or computerized tomography (CT scans). These enable your doctor to examine internal photos of your foot.
Treatment Overview
Stress fractures typically heal with rest and home care. However, incidents occurring in odd locations or that produce more severe symptoms may require surgery.
Non-Surgical Treatments
In many cases, the first line of treatment is a first aid practice called RICE. This acronym is short for (R) rest, (I) icing the impacted bone, (C) compressing it so that it cannot shift and incur further damage, and (E) elevating the foot over your heart, which stimulates blood circulation to the region.
Other non-surgical remedies include remaining off the injured foot for six to eight weeks for complete healing. Stress fractures may need a bracing device like a cast.
Surgical Interventions
Surgery often centers around the insertion of stabilizing devices. Typically, they are made of strong materials and are designed to keep impacted bones in place until the healing process is complete.
ANKLE SPRAINS
Anatomy
The ankle is a major joint that connects critical foot and leg bones together. These bones are connected to muscles and other structures by soft tissues called ligaments.
Description
Ankle sprains occur when the ligaments either stretch or, in more severe instances, tear.
Causes
Ankle sprains can result from several causes, including exercising on uneven pavement, acute traumatic force, falls that cause the ankle to twist, and competitions that require your ankle to roll, turn and twist repeatedly.
Symptoms
The symptoms you experience will depend upon the sprain’s severity. Sprains are labeled Grades One, Two, or Three. Lower-grade sprains might lead to occurrences like:
- Pain in the impacted ankle.
- Swelling.
- Bruising.
- Pain when touching and placing any object, even something as soft as a sock, on top of the area.
In more severe instances, you might witness some or all the events mentioned above, plus mobility issues, difficulty placing weight on the impacted foot, and instability.
Diagnosis
Ankle sprains usually produce telltale symptoms that often lead your doctor to a diagnosis. But your doctor may might test your range of motion and stability and use imaging tests to confirm ligament damage.
Treatment Overview
Less severe sprains usually respond to non-surgical care. However, severe soft tissue damage may require operative procedures.
Non-Surgical Treatments
Mild Grade One events may favorably respond to RICE therapy. Additional treatment options might include the use of crutches, joint stabilization in casts or other movement-restricting apparatuses, the use of pain and inflammation-reducing medications, and physical therapy to maintain your ankle’s strength and motion range.
Surgical Efforts
In the rare circumstance that surgery must be performed, the two most common surgeries are arthroscopy and reconstruction.
Arthroscopic surgery is conducted using a camera. Surgeons insert a tiny camera into your ankle and use small instruments to detach parts of the torn ligament caught in the joint. During the reconstruction process, the torn ligament is repaired and stitched.
ACHILLES TENDINITIS
Anatomy
The body’s largest tendon is the Achilles tendon, named for the famous figure in Greek mythology. It connects the heel bone to your lower leg muscles.
Description
Tendonitis occurs when the Achilles tendon becomes inflamed.
Causes
The condition is often the result of overuse or injury. Sports requiring increased leg bending, running, or jumping increase the risk. Other precipitating factors include poor conditioning techniques like:
- Failing to stretch before exercising.
- A sudden increase in the amount of exercise performed.
- The intensity with which the workload is undertaken.
Symptoms
Like most physical injuries, the most common symptom is pain. Such discomfort is usually worse in the morning and worsens following physical activity. There may also be a thickening of the tendon and swelling.
Diagnosis
Inflammation can occur at any point along the tendon. Therefore, your doctor will perform a visible examination of the back of your leg and check for any of the previously mentioned symptoms. Imaging tests may be performed to rule out other causes.
Treatment Overview
In most uncomplicated cases, home care should bring about a full recovery. However, if typical treatments fail to work or pain lingers for more than six months, surgery might be needed.
Non-Surgical Remedies
Initial treatment often includes the RICE protocol followed by orthotic implementation, physical therapy, and corticosteroid injections.
Surgical Intervention for a torn ligament
Two types of operations are usually undertaken to correct Achilles tendonitis – gastrocnemius recession and debridement.
Gastrocnemius recession lengthens the calf muscles to help alleviate the pressure placed on the Achilles tendon.
During debridement, the injured portion of the tendon is removed and stitched. Sometimes debridement also involves tendon transfer. Tendon transfer is when portions of a ligament (found elsewhere in the body or created from synthetic materials) are inserted to fill the space of the voided tendon.
Next Steps
If you have been diagnosed with any of these sports foot injuries or are experiencing the symptoms of such conditions, please contact us. Talk to your Florida Orthopaedic Institute physician today to learn more about sports foot injuries.
Areas of Focus
- Foot, Ankle & Lower Leg
- Achilles Tendinitis - Achilles Insertional Calcific Tendinopathy (ACIT)
- Achilles Tendon Rupture
- Achilles Tendonitis
- Ankle Fracture Surgery
- Ankle Fractures (Broken Ankle)
- Ankle Fusion Surgery
- Arthroscopic Articular Cartilage Repair
- Arthroscopy Of the Ankle
- Bunions
- Charcot Joint
- Common Foot Fractures in Athletes
- Foot Stress Fractures
- Hallux Rigidus Surgery - Cheilectomy
- Hammer Toe
- High Ankle Sprain (Syndesmosis Ligament Injury)
- Intraarticular Calcaneal Fracture
- Lisfranc Injuries
- Mallet, Hammer & Claw Toes
- Metatarsalgia
- Morton’s Neuroma
- Neuromas (Foot)
- Orthopedic Physician Or A Podiatrist? Definition of a Podiatrist
- Plantar Fasciitis
- Sports Foot Injuries
- Sprained Ankle
- Total Ankle Replacement
- Turf Toe
The following Florida Orthopaedic Institute physicians specialize in Sports Foot Injuries:
Specialties
- AC Joint Injuries
- Achilles Tendinitis - Achilles Insertional Calcific Tendinopathy (ACIT)
- Achilles Tendon Rupture
- Achilles Tendonitis
- ACL Injuries
- Ankle Fracture Surgery
- Ankle Fractures (Broken Ankle)
- Ankle Fusion Surgery
- Anterior Cervical Corpectomy & Discectomy
- Arthroscopic Articular Cartilage Repair
- Arthroscopic Chondroplasty
- Arthroscopic Debridement of the Elbow
- Arthroscopy Of the Ankle
- Articular Cartilage Restoration
- Artificial Disk Replacement (ADR)
- Aspiration of the Olecranon Bursa - Fluid In Elbow
- Atraumatic Shoulder Instability
- Avascular Necrosis (Osteonecrosis)
- Bankart Repair
- Basal Joint Surgery
- Bicep Tendon Tear
- Bicep Tenodesis
- Bone Cement Injection
- Bone Growth Stimulation
- Bone Health Clinic
- Broken Collarbone
- Bunions
- Bursitis of the Shoulder (Subacromial Bursitis)
- Calcific Tendinitis of the Shoulder
- Carpal Tunnel Syndrome
- Charcot Joint
- Chiropractic
- Clavicle Fractures
- Colles’ Fractures (Broken Wrist)
- Common Foot Fractures in Athletes
- Community Outreach
- Cubital Tunnel Syndrome
- De Quervain's Tenosynovitis
- Deep Thigh Bruising
- Degenerative Disk Disease
- Diffuse Idiopathic Skeletal Hyperostosis (DISH)
- Discectomy
- Discitis Treatment & Information
- Dislocated Shoulder
- Dupuytren’s Disease
- Elbow
- Elbow Bursitis
- Elbow Injuries & Inner Elbow Pain in Throwing Athletes
- Epidural Injections for Spinal Pain
- Finger Dislocation
- Flexor Tendonitis
- Foot Stress Fractures
- Foot, Ankle & Lower Leg
- Foraminotomy
- Fractured Fingers
- Fractures Of The Shoulder Blade (Scapula)
- Fractures Of The Tibial Spine
- Functional Nerve Transfers of The Hand
- Ganglion Cysts
- General Orthopedics
- Glenoid Labrum Tear
- Golfer's Elbow
- Groin Strains and Pulls
- Growth Plate Injuries Of The Elbow
- Hallux Rigidus Surgery - Cheilectomy
- Hammer Toe
- Hamstring Injuries
- Hand & Finger Replantation
- Hand & Wrist
- Hand Nerve Decompression
- Hand Skin Grafts
- Hand, Wrist, Elbow & Shoulder
- Heat Injury/Heat Prostration
- High Ankle Sprain (Syndesmosis Ligament Injury)
- Hip & Thigh
- Hip Arthroscopy
- Hip Dislocation
- Hip Flexor Strains
- Hip Fractures
- Hip Hemiarthroplasty
- Hip Impingement Labral Tears
- Hip Muscle Strains
- Hip Pointers and Trochanteric Bursitis
- Hyperextension Injury of the Elbow
- Iliopsoas Tenotomy
- Iliotibial Band Syndrome
- Impingement Syndrome of the Shoulder
- Interlaminar Implants
- Interlaminar Lumbar Instrumental Fusion: ILIF
- Interventional Pain Management
- Interventional Spine
- Intraarticular Calcaneal Fracture
- Joint Replacement
- Knee & Leg
- Kyphoplasty (Balloon Vertebroplasty)
- Kyphosis
- Labral Tears Of The Hip (Acetabular Labrum Tears)
- Laminectomy: Decompression Surgery
- Lateral Collateral Ligament (LCL) Injuries
- Lisfranc Injuries
- Little League Shoulder
- LITTLE LEAGUER'S ELBOW (MEDIAL APOPHYSITIS)
- Lumbar Epidural Steroid Injection
- Lumbar Interbody Fusion (IBF)
- MACI
- Mallet, Hammer & Claw Toes
- Medial Collateral Ligament Injuries
- Meniscus Tears
- Metatarsalgia
- Minimally Invasive Spine Surgery
- Morton’s Neuroma
- Muscle Spasms
- Muscle Strains of The Calf
- Nerve Pain
- Neuromas (Foot)
- Neurosurgery
- Olecranon Stress Fractures
- Orthopaedic Total Wellness
- Orthopaedic Trauma
- Orthopedic Physician Or A Podiatrist? Definition of a Podiatrist
- Osteoarthritis of the Hip
- Osteoporosis
- Outpatient Spine Surgery
- Partial Knee Replacement
- Patellar Fracture
- Pelvic Ring Fractures
- Peripheral Nerve Surgery (Hand) Revision
- Pinched Nerve
- Piriformis Syndrome
- Piriformis Syndrome
- Plantar Fasciitis
- Plastic Surgery
- Podiatry
- Primary Care Sports Medicine
- Quadriceps Tendon Tear
- Radial Tunnel Syndrome (Entrapment of the Radial Nerve)
- Revascularization of the Hand
- Reverse Total Shoulder Replacement
- Rheumatoid Arthritis (RA) of the Shoulder
- Rheumatoid Arthritis Of The Hand
- Robotics
- Rotator Cuff Tears
- Runner's Knee
- Sacroiliac Joint Pain
- Sciatica
- Scoliosis
- Senior Strong
- Shin Splints
- Shoulder
- Shoulder Arthritis
- Shoulder Arthroscopy
- Shoulder Injury: Pain In The Overhead Athlete
- Shoulder Replacement
- Shoulder Separations
- Shoulder Socket Fracture (Glenoid Fracture)
- SLAP Tears & Repairs
- Spinal Fusion
- Spine
- Spondylolisthesis and Spondylolysis
- Sports Foot Injuries
- Sports Hernias (Athletic Pubalgia)
- Sports Medicine
- Sports Wrist and Hand Injuries
- Sprained Ankle
- Sprained Wrist Symptoms and Treatment
- Subacromial Decompression
- Sudden (Acute) Finger, Hand & Wrist Injuries
- Targeted Muscle Reinnervation (TMR)
- Tendon Transfers of The Hand
- Tennis Elbow Treatment
- Thigh Fractures
- Thigh Muscle Strains
- Thumb Ulnar Collateral Ligament Injuries
- Total Ankle Replacement
- Total Hip Arthroplasty
- Total Hip Replacement - Anterior Approach
- Total Knee Replacement Surgery
- Trapezius Strain (Muscle Strain of The Upper Back)
- Traumatic Shoulder Instability
- Tricep Pain & Tendonitis
- Trigger Finger
- Turf Toe
- UCL (Ulnar Collateral Ligament) Injuries
- Ulnar Neuritis
- Valgus Extension Overload
- Vertebroplasty
- WALANT (Wide Awake Local Anesthesia No Tourniquet)
- Whiplash and Whiplash Associated Disorder (WAD)
- Wound Care
- Wrist Arthroscopy
- Wrist Fractures
- Wrist Tendonitis
Services
- Physical Medicine & Rehabilitation
- Physical Therapy
- Primary Care Sports Medicine
- PROMs (Patient-Reported Outcome Measures)
- Same-Day Orthopaedic Appointments Now Available
- Sports Medicine
- Sports-Related Concussion Treatment
- Telehealth Page
- Telemedicine
- Workers' Compensation
- Workers' Compensation Dispensary
- X-Ray
