Torn Achilles Tendon
OVERVIEW
An Achilles tendon rupture is when the Achilles tendon is torn. This tear usually occurs when sudden, extreme stress is applied to the tendon, causing it to tear. The tear can be either partial or complete, and can be treated surgically or non-surgically, depending on the severity of the tear. Both treatment types need to be paired with physical therapy exercises to return to former activity levels.
ANATOMY
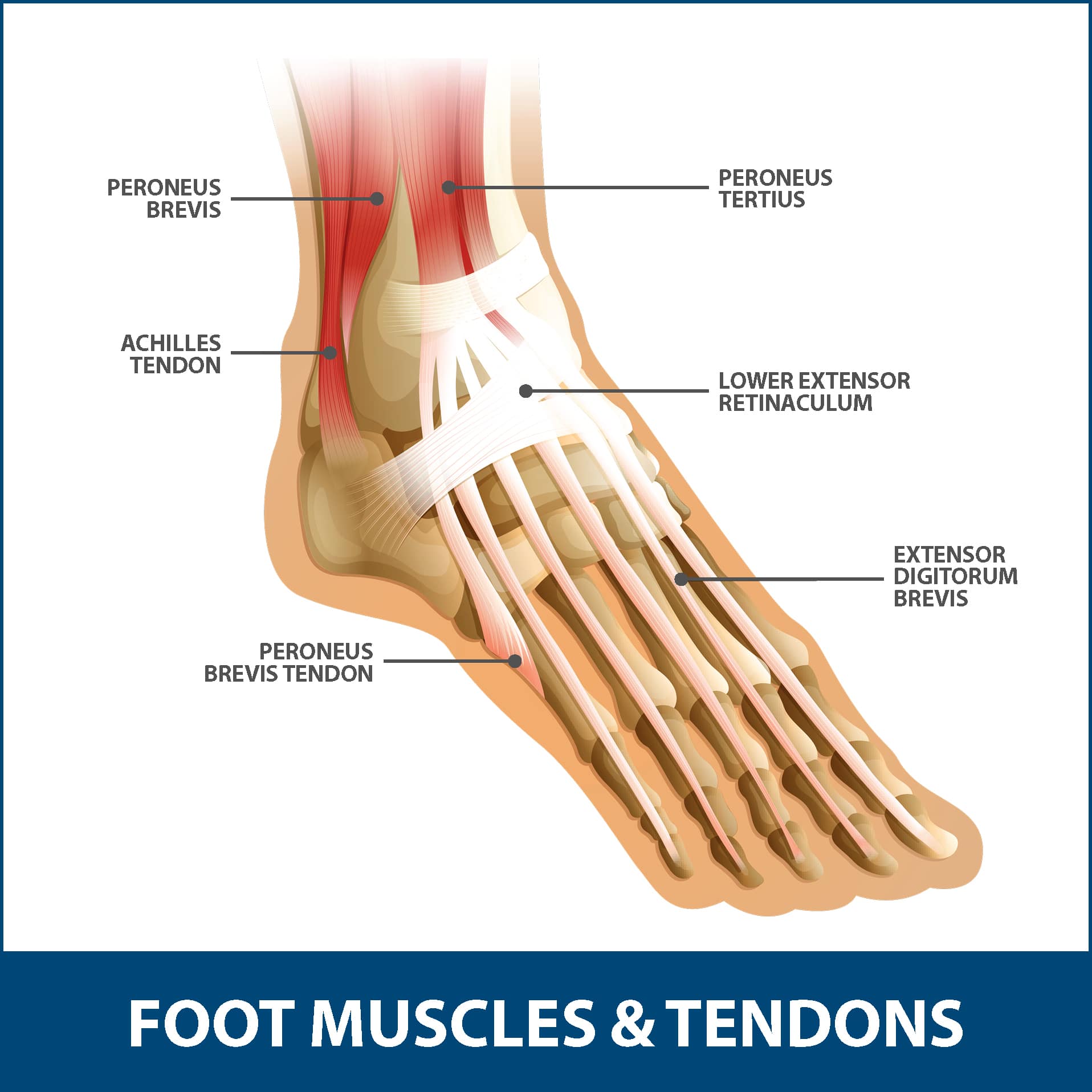
The Achilles tendon, also known as the calcaneal tendon, is a tough, fibrous band of tissue that connects the calf muscle to the heel bone (calcaneus). When the calf muscles flex, the Achilles tendon pulls on the heel, allowing us to walk, run, climb stairs, jump, and stand on the tip of your toes. It is both the strongest and largest tendon in the entire body. While it may be the strongest, it is also vulnerable to injury, due to the high tensions placed on it and its limited blood supply. The tearing of the Achilles tendon is when the tendon tears, resulting in the separation of the tendon fibers. When this occurs, the tendon can no longer perform its normal function.
DESCRIPTION
An Achilles tendon rupture is when the Achilles tendon is torn. The tear may be either partial or complete. In the case of a partial tear, the tendon is partially torn but still joined to the calf muscle. During a complete tear, the connection between the calf muscle and the ankle bone is completely lost. Ruptures are often caused by a sudden increase in stress on the Achilles tendon, such as falling from a height, the intensity of sports, or falling into a hole. While an Achilles tendon rupture can happen to anyone, certain factors increase the likelihood of experiencing the injury:
- Age. The peak age for a torn Achilles tendon is 30 to 40.
- Sex. Men are up to five times more likely to experience an Achilles tendon rupture than women.
- Recreational sports. People who take part in recreational sports, specifically ones that involve running, jumping, and sudden starts and stops, have an increased chance of experiencing an Achilles tendon rupture.
- Steroid injections. Doctors sometimes inject steroids into an ankle joint to reduce pain and inflammation. This medication can weaken nearby tendons and has been associated with Achilles tendon ruptures.
- Certain antibiotics. Fluoroquinolone antibiotics, such as levofloxacin (Levaquin) or ciprofloxacin (Cipro), increase the risk of Achilles tendon ruptures.
- Obesity. Excess weight puts more strain on the tendon.

SYMPTOMS
While it is possible to experience no symptoms with an Achilles tendon rupture, most people experience the following:
- The feeling of having been kicked in the calf.
- Pain (possibly severe).
- Swelling near the heel.
- Inability to bend the foot downward or “push off” the injured leg when walking.
- Inability to stand on the toes of the injured leg.
- Popping or snapping sound during the moment of injury.

DIAGNOSIS
Your Florida Orthopaedic Institute physician will look at your lower leg for tenderness, swelling, and a possible gap in your tendon if it has ruptured completely. Your physician may also squeeze your calf muscle to see if it will automatically flex. If it does not, there is a high chance your Achilles tendon has ruptured. If these tests do not accurately depict whether the tendon has torn partially or completely, then an MRI or ultrasound may be ordered. Both of these tests create images of the tissues of your body and show the tendon.
TREATMENT (OVERVIEW)
Both surgical and nonsurgical treatments are available for the repair of an Achilles tendon rupture. While surgery is often performed to repair the rupture, non-surgical options work well for less severe cases.
NONSURGICAL TREATMENTS
Nonsurgical treatments generally include:
- Resting the tendon by using crutches.
- Icing the area.
- Pain relievers.
- Preventing the ankle from moving for the first few weeks usually with the use of a walking boot with heel wedges or a cast with the foot flexed down.
While nonsurgical options avoid the risks associated with surgery, such as infection, a nonsurgical approach may increase your chances of re-rupture. Additionally, a full recovery may take longer to achieve with nonsurgical treatments.
SURGICAL PROCEDURES/TREATMENTS
The surgical procedure generally involves making an incision in the back of the lower leg and stitching the torn tendon together. Depending on the severity of the rupture, the repair might be reinforced with other tendons, usually ones from other parts of the foot. Patients are generally released from the hospital the day of surgery.
This surgery should not be performed on a patient with an active infection or unhealthy skin at or around the site of the Achilles tendon rupture, or if they are not healthy enough to undergo surgery.
NEXT STEPS
After either a surgical or nonsurgical approach, physical therapy exercises will be required to strengthen the leg muscles and the Achilles tendon. Most people return to their former level of activity within four to six months. It is important to continue strength and stability training afterwards because some problems can persist for up to a year. Currently, rehabilitation after either surgical or nonsurgical treatments is progressing to be done earlier. Studies are ongoing in this area to determine its safety and effectiveness.
Your Florida Orthopaedic Institute physician is sub-specialty trained and up to date on the latest treatment methods and procedures. Schedule an appointment if you think you have injured your Achilles tendon.
Areas of Focus
- Foot, Ankle & Lower Leg
- Achilles Tendinitis - Achilles Insertional Calcific Tendinopathy (ACIT)
- Achilles Tendon Rupture
- Achilles Tendonitis
- Ankle Fracture Surgery
- Ankle Fractures (Broken Ankle)
- Ankle Fusion Surgery
- Arthroscopic Articular Cartilage Repair
- Arthroscopy Of the Ankle
- Bunions
- Charcot Joint
- Common Foot Fractures in Athletes
- Foot Stress Fractures
- Hallux Rigidus Surgery - Cheilectomy
- Hammer Toe
- High Ankle Sprain (Syndesmosis Ligament Injury)
- Intraarticular Calcaneal Fracture
- Lisfranc Injuries
- Mallet, Hammer & Claw Toes
- Metatarsalgia
- Morton’s Neuroma
- Neuromas (Foot)
- Orthopedic Physician Or A Podiatrist? Definition of a Podiatrist
- Plantar Fasciitis
- Sports Foot Injuries
- Sprained Ankle
- Total Ankle Replacement
- Turf Toe
The following Florida Orthopaedic Institute physicians specialize in Achilles Tendon Rupture:
Specialties
- AC Joint Injuries
- Achilles Tendinitis - Achilles Insertional Calcific Tendinopathy (ACIT)
- Achilles Tendon Rupture
- Achilles Tendonitis
- ACL Injuries
- Ankle Fracture Surgery
- Ankle Fractures (Broken Ankle)
- Ankle Fusion Surgery
- Anterior Cervical Corpectomy & Discectomy
- Arthroscopic Articular Cartilage Repair
- Arthroscopic Chondroplasty
- Arthroscopic Debridement of the Elbow
- Arthroscopy Of the Ankle
- Articular Cartilage Restoration
- Artificial Disk Replacement (ADR)
- Aspiration of the Olecranon Bursa - Fluid In Elbow
- Atraumatic Shoulder Instability
- Avascular Necrosis (Osteonecrosis)
- Bankart Repair
- Basal Joint Surgery
- Bicep Tendon Tear
- Bicep Tenodesis
- Bone Cement Injection
- Bone Growth Stimulation
- Bone Health Clinic
- Broken Collarbone
- Bunions
- Bursitis of the Shoulder (Subacromial Bursitis)
- Calcific Tendinitis of the Shoulder
- Carpal Tunnel Syndrome
- Charcot Joint
- Chiropractic
- Clavicle Fractures
- Colles’ Fractures (Broken Wrist)
- Common Foot Fractures in Athletes
- Community Outreach
- Cubital Tunnel Syndrome
- De Quervain's Tenosynovitis
- Deep Thigh Bruising
- Degenerative Disk Disease
- Diffuse Idiopathic Skeletal Hyperostosis (DISH)
- Discectomy
- Discitis Treatment & Information
- Dislocated Shoulder
- Dupuytren’s Disease
- Elbow
- Elbow Bursitis
- Elbow Injuries & Inner Elbow Pain in Throwing Athletes
- Epidural Injections for Spinal Pain
- Finger Dislocation
- Flexor Tendonitis
- Foot Stress Fractures
- Foot, Ankle & Lower Leg
- Foraminotomy
- Fractured Fingers
- Fractures Of The Shoulder Blade (Scapula)
- Fractures Of The Tibial Spine
- Functional Nerve Transfers of The Hand
- Ganglion Cysts
- General Orthopedics
- Glenoid Labrum Tear
- Golfer's Elbow
- Groin Strains and Pulls
- Growth Plate Injuries Of The Elbow
- Hallux Rigidus Surgery - Cheilectomy
- Hammer Toe
- Hamstring Injuries
- Hand & Finger Replantation
- Hand & Wrist
- Hand Nerve Decompression
- Hand Skin Grafts
- Hand, Wrist, Elbow & Shoulder
- Heat Injury/Heat Prostration
- High Ankle Sprain (Syndesmosis Ligament Injury)
- Hip & Thigh
- Hip Arthroscopy
- Hip Dislocation
- Hip Flexor Strains
- Hip Fractures
- Hip Hemiarthroplasty
- Hip Impingement Labral Tears
- Hip Muscle Strains
- Hip Pointers and Trochanteric Bursitis
- Hyperextension Injury of the Elbow
- Iliopsoas Tenotomy
- Iliotibial Band Syndrome
- Impingement Syndrome of the Shoulder
- Interlaminar Implants
- Interlaminar Lumbar Instrumental Fusion: ILIF
- Interventional Pain Management
- Interventional Spine
- Intraarticular Calcaneal Fracture
- Joint Replacement
- Knee & Leg
- Kyphoplasty (Balloon Vertebroplasty)
- Kyphosis
- Labral Tears Of The Hip (Acetabular Labrum Tears)
- Laminectomy: Decompression Surgery
- Lateral Collateral Ligament (LCL) Injuries
- Lisfranc Injuries
- Little League Shoulder
- LITTLE LEAGUER'S ELBOW (MEDIAL APOPHYSITIS)
- Lumbar Epidural Steroid Injection
- Lumbar Interbody Fusion (IBF)
- MACI
- Mallet, Hammer & Claw Toes
- Medial Collateral Ligament Injuries
- Meniscus Tears
- Metatarsalgia
- Minimally Invasive Spine Surgery
- Morton’s Neuroma
- Muscle Spasms
- Muscle Strains of The Calf
- Nerve Pain
- Neuromas (Foot)
- Neurosurgery
- Olecranon Stress Fractures
- Orthopaedic Total Wellness
- Orthopaedic Trauma
- Orthopedic Physician Or A Podiatrist? Definition of a Podiatrist
- Osteoarthritis of the Hip
- Osteoporosis
- Outpatient Spine Surgery
- Partial Knee Replacement
- Patellar Fracture
- Pelvic Ring Fractures
- Peripheral Nerve Surgery (Hand) Revision
- Pinched Nerve
- Piriformis Syndrome
- Piriformis Syndrome
- Plantar Fasciitis
- Plastic Surgery
- Podiatry
- Primary Care Sports Medicine
- Quadriceps Tendon Tear
- Radial Tunnel Syndrome (Entrapment of the Radial Nerve)
- Revascularization of the Hand
- Reverse Total Shoulder Replacement
- Rheumatoid Arthritis (RA) of the Shoulder
- Rheumatoid Arthritis Of The Hand
- Robotics
- Rotator Cuff Tears
- Runner's Knee
- Sacroiliac Joint Pain
- Sciatica
- Scoliosis
- Senior Strong
- Shin Splints
- Shoulder
- Shoulder Arthritis
- Shoulder Arthroscopy
- Shoulder Injury: Pain In The Overhead Athlete
- Shoulder Replacement
- Shoulder Separations
- Shoulder Socket Fracture (Glenoid Fracture)
- SLAP Tears & Repairs
- Spinal Fusion
- Spine
- Spondylolisthesis and Spondylolysis
- Sports Foot Injuries
- Sports Hernias (Athletic Pubalgia)
- Sports Medicine
- Sports Wrist and Hand Injuries
- Sprained Ankle
- Sprained Wrist Symptoms and Treatment
- Subacromial Decompression
- Sudden (Acute) Finger, Hand & Wrist Injuries
- Targeted Muscle Reinnervation (TMR)
- Tendon Transfers of The Hand
- Tennis Elbow Treatment
- Thigh Fractures
- Thigh Muscle Strains
- Thumb Ulnar Collateral Ligament Injuries
- Total Ankle Replacement
- Total Hip Arthroplasty
- Total Hip Replacement - Anterior Approach
- Total Knee Replacement Surgery
- Trapezius Strain (Muscle Strain of The Upper Back)
- Traumatic Shoulder Instability
- Tricep Pain & Tendonitis
- Trigger Finger
- Turf Toe
- UCL (Ulnar Collateral Ligament) Injuries
- Ulnar Neuritis
- Valgus Extension Overload
- Vertebroplasty
- WALANT (Wide Awake Local Anesthesia No Tourniquet)
- Whiplash and Whiplash Associated Disorder (WAD)
- Wound Care
- Wrist Arthroscopy
- Wrist Fractures
- Wrist Tendonitis
Services
- Physical Medicine & Rehabilitation
- Physical Therapy
- Primary Care Sports Medicine
- PROMs (Patient-Reported Outcome Measures)
- Same-Day Orthopaedic Appointments Now Available
- Sports Medicine
- Sports-Related Concussion Treatment
- Telehealth Page
- Telemedicine
- Workers' Compensation
- Workers' Compensation Dispensary
- X-Ray
