Total Ankle Replacement Surgery
Leaders in Total Ankle Replacement
With over 20 years of experience, performing thousands of ankle fusions, triple arthrodeses, subtalar fusions and over 300 total ankle replacements, Florida Orthopaedic Institute surgeons are leaders in the field.
In 1995, the Agility® total ankle prosthesis became available in the U.S. Florida Orthopaedic Institute was the third center in the country to implant this device, with surgeons involved in design, teaching, and evaluation of the implant. Later that year a European ankle replacement known as the S.T.A.R.® was released, and again Florida Orthopaedic Institute surgeons were involved in the first trial of that prosthesis in the U.S. Since that time, the foot and ankle surgeons at Florida Orthopaedic Institute (all trained on total ankle replacements) have performed hundreds of replacements.
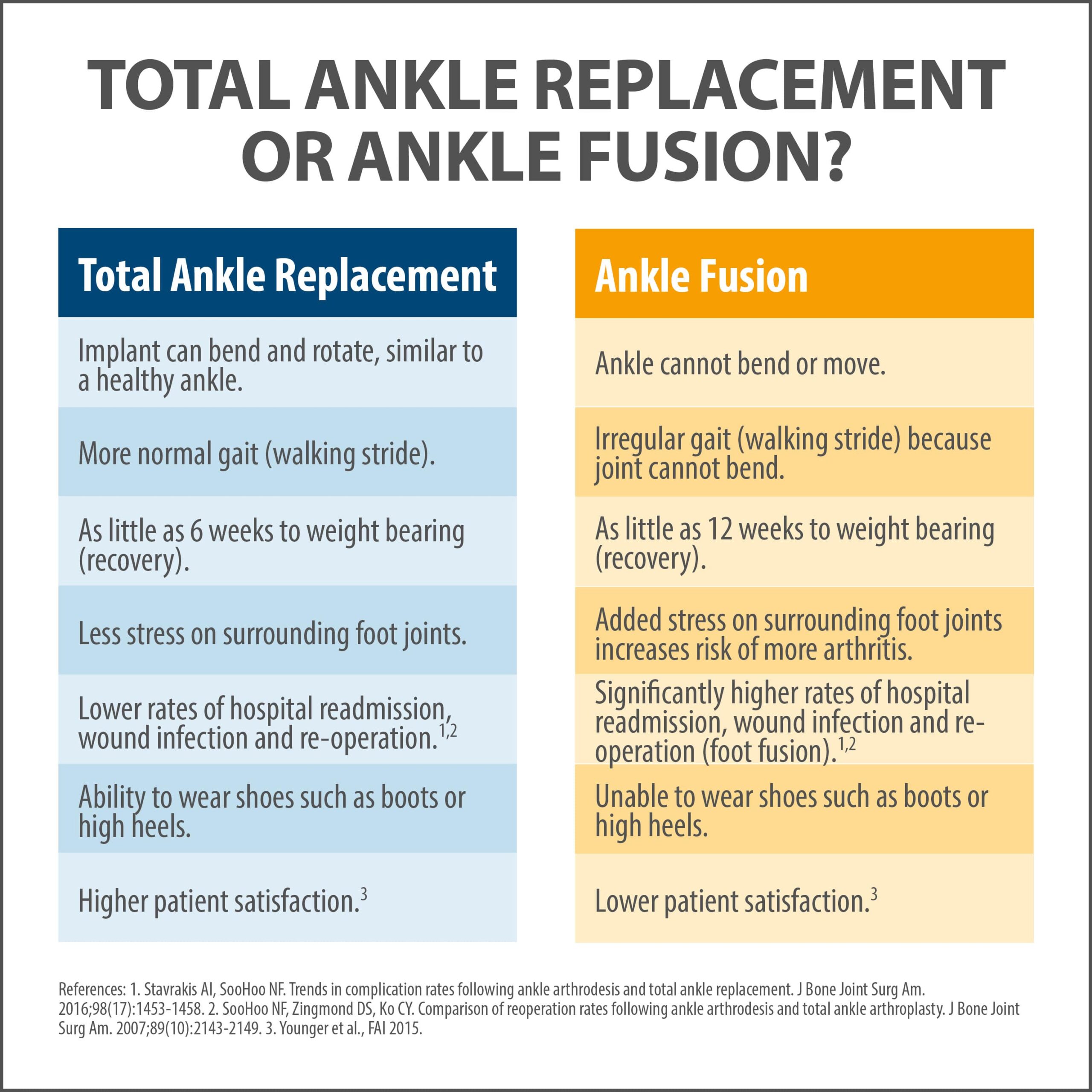
For those patients that are not candidates for an ankle replacement, ankle fusions remain the gold standard. Patients can walk without a limp using modern techniques to remove minimal amounts of bone and position the ankle so the joint below moves well.
Because of the combined expertise of the foot and ankle surgeons, as well as their national reputation, patients are referred not only locally, but from all over the country. Many of the referrals are patients with significant post-surgical complications including infections, failed joint replacements, poorly positioned fusions, and non-healed fractures. These patients are sent to Florida Orthopaedic Institute for definitive solutions to their problems, and in most cases surgeons are able to improve their lives. This ability to solve complex problems and help patients is the driving force behind maintaining the high quality of care offered, and why Florida Orthopaedic Institute is a regional and national referral center.
Recognized as a WRIGHT Innovation Center
As a recognized Wright Innovation Center, Florida Orthopaedic Institute surgeons are highly experienced in performing the MOVERIGHT™ Total Ankle Replacement procedure.
- The highest volume Ankle Replacement Center in the state.
- The first to perform total ankle replacements in Florida.
- Leaders in bringing Total Ankle Replacement to Florida.
In the Southeast and most certainly in Florida, the physicians at Florida Orthopaedic Institute have had an enormous impact on total ankle replacements. By far, they perform the most total ankle replacement surgeries in Florida. These surgeons are hundreds of replacement cases ahead of any competition in the state.
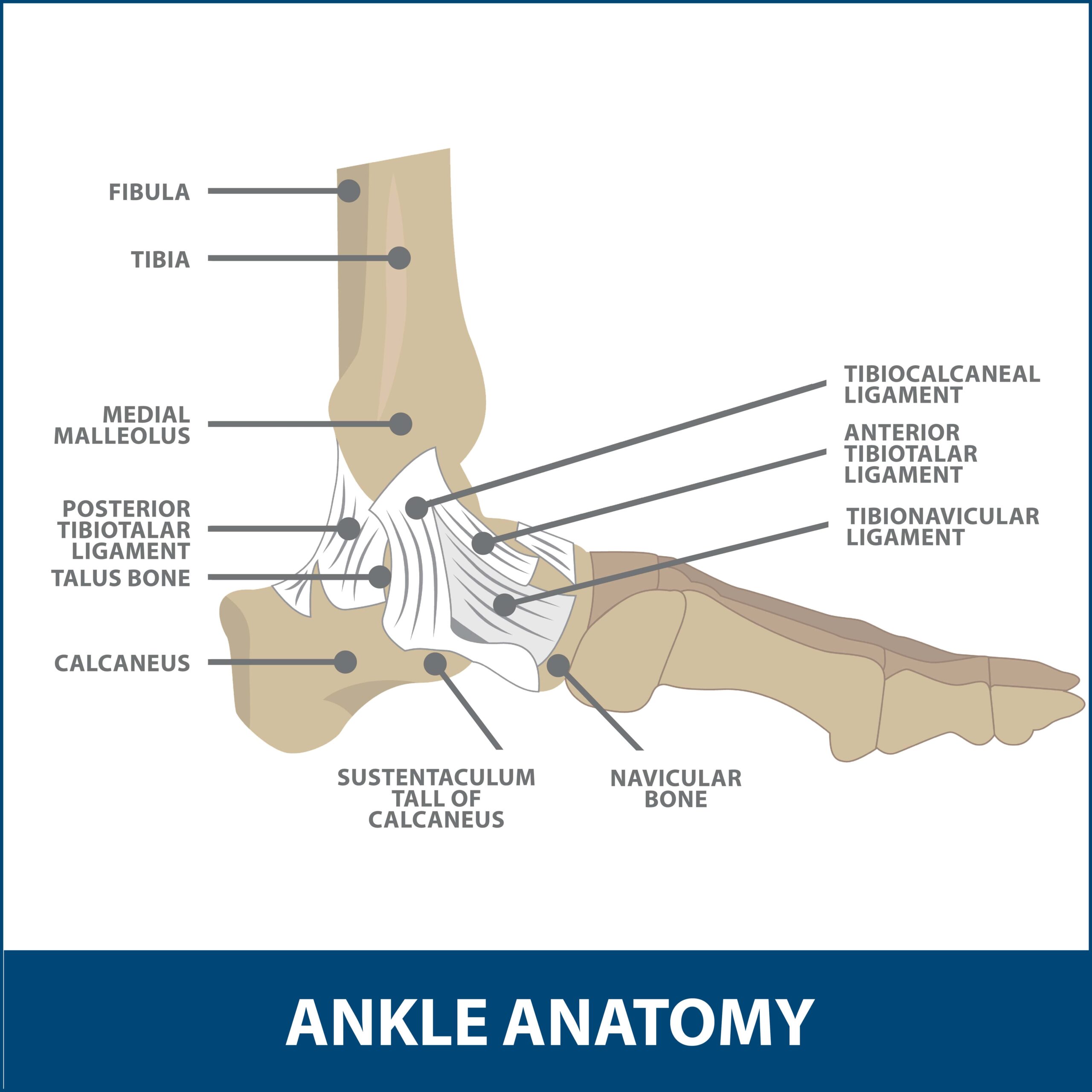
Anatomy of the Ankle
The human ankle joint is formed by three bones and acts like a hinge. The ankle bone (the talus) fits inside a socket formed by the lower end of the tibia (the shinbone), and the small bone of the lower leg (the fibula). The bottom of the talus sits on the heel bone (the calcaneus). A normal ankle can move forwards, from side-to-side, and twist, and is one of the most flexible, free-moving joints in the body.

The ankle contains cartilage which absorbs shock like other free-moving joints. It is held together with straps of tough tissue (ligaments), which help keep the joint together. The ankle joint depends on the successful coordination of many interrelated parts including bones, muscles, tendons, ligaments, and nerves. With arthritis, the cartilage in the joint wears down, resulting in bone-on-bone contact, causing pain and limited activity, and is one of the most common reasons for ankle replacement surgery.

Benefits of Total Ankle Replacement
After evaluating your situation and trying other surgical and non-surgical procedures, your surgeon may offer you ankle replacement surgery. Benefits include the relief of pain and return of function to the ankle. The INFINITY® Total Ankle gives a patient more mobility by reducing pain, restoring alignment and replacing the flexion and extension movement in the ankle joint. It is designed for patients with ankle joints damaged by severe rheumatoid, post-traumatic, or degenerative arthritis. After surgery, patients are usually pain-free, sometimes the first time in years. They can walk normally with their foot straight and without a limp. For many, this is the first time in their life where they’ve had normal mobility and find the experience profoundly life-changing.
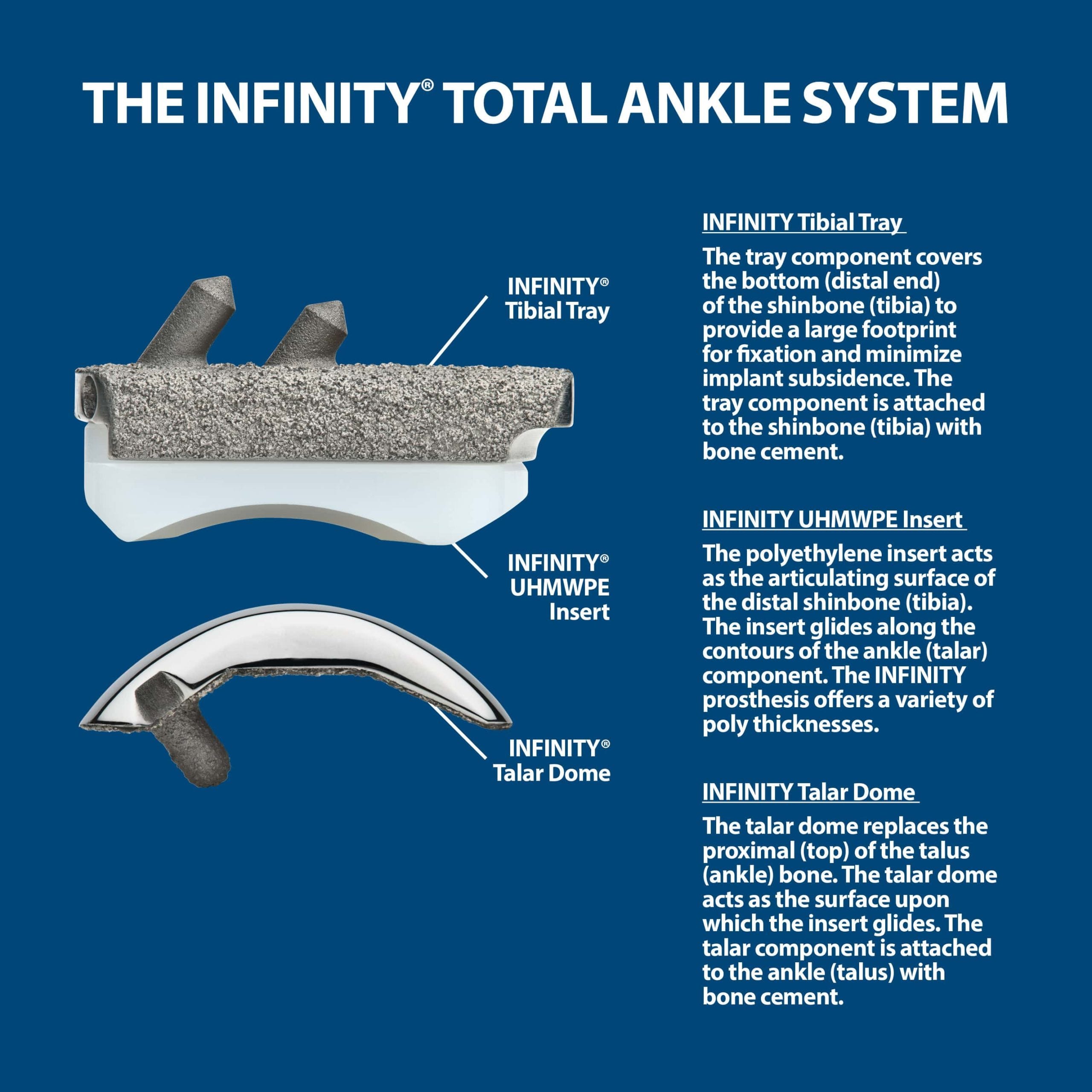
The Infinity® Total Ankle System
The INFINITY Total Ankle System consists of a highly polished metal talar dome, a titanium alloy tibial tray, and an ultra-high molecular weight polyethylene insert (UHMWPE). All components are available in varying sizes to best match a patient’s anatomy.
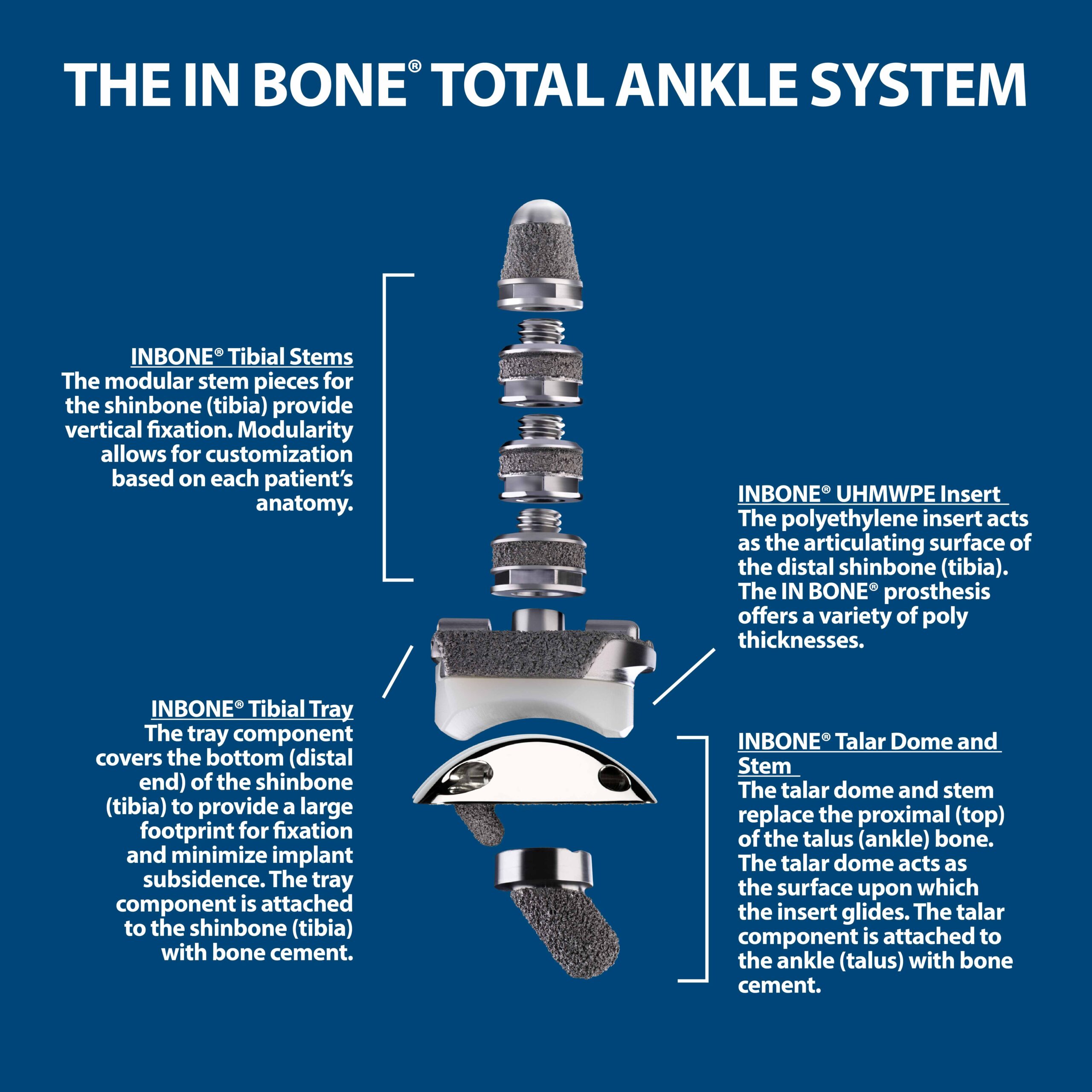
The INBONE® Total Ankle System
The INBONE® Total Ankle System consists of a talar dome with a modular talar stem, a tibial tray, a four-component tibial stem assembly that attaches to the tibial tray, and an ultrahigh molecular weight polyethylene insert (UHMWPE). Components are available in varying sizes to best match your anatomy.
Prophecy® Navigation
PROPHECY Preoperative Navigation Guides are key components in total ankle replacement. Using a combination of computer imaging and a CT scan, a customized plan is developed for your unique anatomy, before ankle replacement surgery.
PROPHECY guides provide the alignment accuracy of INFINITY and IN BONE Total Ankle Systems while reducing surgical steps. Crucial anatomic landmarks are identified before surgery with patient-specific instrumentation, and there is less radiation exposure from x-rays during surgery.
THINGS YOU SHOULD KNOW
Not everyone is a good candidate for the total ankle replacement. Your Florida Orthopaedic surgeon will discuss your lifestyle and health to determine if total ankle replacement surgery is the right option for you.
Diseases of the Ankle
- Osteoarthritis
- Osteoarthritis (also known as degenerative arthritis), is the most common joint disorder, caused by aging and wear and tear on a joint.
- Rheumatoid Arthritis
- When the body’s immune system attacks the synovial lining of the joints, as it would attack foreign bacteria, rheumatoid arthritis occurs. Synovial fluid is the clear, smooth, oil-like lubricating liquid that makes it easier for joints to move.
- Tarsal Tunnel Syndrome
- Tarsal Tunnel Syndrome is the result of nerve compression in the ankle where the sensory nerve passes under the tarsal tunnel. When the tunnel is irritated by pressure, the result is numbness and tingling in the foot and ankle.
- Ankle Injury
- Ankle injury occurs when injury (trauma) has occurred to the ankle joint. Ankle injuries can cause swelling, pain, weakness, and difficulty walking, and significantly affect mobility.
Alternatives to Ankle Replacement
There are several non-surgical alternatives to ankle replacement surgery. Many of the nonsurgical methods provide relief because they limit motion, which decreases the irritation of the arthritic joint. Shoe inserts (orthotics), such as pads and arch supports, are one method. Ankle braces and canes take the pressure and stress off the arthritic joint. Custom-made shoes with a stiff sole and a rocker bottom (ankle foot orthosis-AFO) decrease motion of the ankle joint.
Direct injections of medication into arthritic joints can give months of pain relief. Body weight control is also key to decreasing stress on the ankle. Although none of these treatments can reverse or cure deteriorated cartilage, they can provide improved function and decreased pain.
If the non-surgical treatments don’t reduce pain sufficiently, surgical options are available. Specific surgery depends on the extent and pattern of cartilage damage and level of ankle pain. Alternatives to ankle replacement include:
DEBRIDEMENT – Cleaning the ankle joint by removing the inflamed joint lining (synovial tissue), loose cartilage fragments and bone spurs (osteophytes). It is done arthroscopically or through open surgery. If the ankle still has a reasonable amount of normal cartilage remaining, debridement can provide pain relief of pain for several months to years.
CADAVER (ALLOGRAFT) ARTHROPLASTY – Cadaver donated cartilage and bone is transplanted into the ankle to replace areas of damaged cartilage.
DISTRACTION ARTHROPLASTY – The ankle is debrided, and then a wire frame is applied thru the bones above and below the ankle. This wire frame holds the ankle stiff and slightly separated, to allow cartilage healing.
FUSION (ARTHRODESIS) – in ankles with dispersed cartilage loss, fusion (arthrodesis) is a procedure where an orthopedic surgeon removes the remaining cartilage and uses screws and other metal hardware to stabilize the joint, allowing the bone to heal together and eliminate motion and pain. The procedure is done externally or internally. In external fixation, surgical pins are fixed inside the leg and ankle bones to keep the bones in place, and an outer metal rod and pins hold the bones in place until they heal. In an internal fixation approach (more common), the cartilage at the ankle joint is removed, and the ankle and leg bones are compressed with internal plates and screws so that the bones fuse.
GLOSSARY OF ANKLE TERMS
Achilles Tendon –the tendon which connects the three strongest flexor muscles of the leg to the foot. A tendon connects the two heads of the gastrocnemius muscle and the deeper soleus muscle to the calcaneus, or heel bone. The tendon can be felt in the back of the ankle, just under the skin, and can be a common source of pain in runners and other athletes. Achilles tendonitis, tendonosis, and rupture are some common tendon problems.
Ankle Instability – Caused by injuries that never heal properly, weak ankle ligaments or heels that tilts inward (varus heel), these are chronic, repetitive sprains of the ankle.
Ankle Joint – The joint between the foot and the lower leg. It allows the foot to move upward (dorsiflex) and move downward (plantarflex). It consists of the two bones of the lower leg (tibia & fibula) and the ankle bone (talus). Ligaments hold the joint together on the inside (deltoid) and outside (lateral ankle ligament complex).
Arthritis – Typically the wearing away of joint surfaces. Arthritis falls into one of three categories: Osteoarthritis: Primary arthritis of the joint and often related to family history. Traumatic arthritis: Arthritis that develops after injury to a joint. Inflammatory arthritis: Occurs when a disease affecting the patient causes the cartilage to wear away. Arthritis treatment is based on the cause and extent of the damage and may include medication, bracing, physical therapy or surgery.
Calcaneus – The heel bone, which consists of two joints. The subtalar joint allows motion of the ankle (talus) bone for inversion and eversion of the foot with the leg. The calcaneocuboid joint controls flexibility of the foot and the arch of the foot with a complex biomechanical function. The Achilles tendon attaches to the back of the calcaneus, and the plantar fascia attaches to the bottom of the calcaneus.
Cartilage – Living tissue that lines the joints. A matrix of proteins and collagen, cartilage is tough, absorbs shock and is very smooth. Healthy cartilage often lasts your whole life without problems. Trauma or disease of the cartilage can cause cartilage cells to die. Joint cartilage cells do not reproduce themselves once our skeletons are fully grown, unlike most tissues in our body. There have been many recent innovations in cartilage transplantation and growth.
Congenital Vertical Talus (CVT) – When the foot is malformed at birth, the ankle bone (talus) is incorrectly formed. This condition frequently requires surgery by an orthopaedic surgeon. The foot may have a reversed arch or “rocker bottom” deformity where the middle of the foot sits lower than the heel and toes.
Cuboid – The midfoot bone on the outside of the foot that lies between the calcaneus and metatarsals. When the midfoot is injured, this bone may be crushed, also known a “Nutcracker fracture”.
Eversion – Twisting out and away from the midline of the body.
Extensor digitorum longus – The foot extensor is a muscle which raises the toes or ankle. The extensor digitorum longus stabilizes the toes against the ground.
Extensor hallucis longus – Stabilizes the joint where the toes meet the foot (first metatarasophalaneal) and forefoot during push-off.
Fibula – Most prominent bone on the outer side of the ankle that also extends to the knee.
Fracture – A bone that has cracked or broken, usually occurring as a result of an injury. In abnormal bone structure, a fracture can occur after a minor injury. Overuse can cause a “stress” fracture. In non-displaced fractures, the pieces of bone don’t separate at all. Displaced fractures have some separation between the broken pieces. Fracture displacement refers to the amount the two broken pieces have moved away from each other. Some bones can heal properly even with a lot of displacement, while some fractured bones need surgery for even a small amount of displacement. Evaluation and treatment by an orthopaedic surgeon are necessary to determine the best course of treatment.
Inflammatory arthritis – Occurs when a disease causes the cartilage to die. Treatment may include medication, bracing or surgery, depending on the cause and extent of the arthritis.
Inversion – Twisting inward, to the midline of the body.
Lateral malleolus – The end of the fibula – the most prominent bone on the outside of the ankle.
Ligament – A band of tissue made primarily of collagen connecting one bone to another, typically supporting a joint. Sprains are injuries to a ligament.
Medial malleolus – Most prominent bone on the inner side of the ankle.
Navicular – A “boat” shaped bone in the midfoot, made up of two joints. The talonavicular joint controls flexibility of the foot and controls the arch of the foot with a complicated biomechanical function. The other joint is the naviculocuneiform joint, which can be injured in midfoot injuries and contributes to flatfoot deformity.
Osteoarthritis – Primary arthritis of a joint. It can be related to family history.
Peroneal tendon – Behind the outside bone of the ankle (the fibula), these two tendons move the foot outwards in a direction called eversion. They balance the ankle and the back of the foot and prevent the foot from turning inwards. They are susceptible to injury as the ankle turns, rolls or becomes sprained because they are not as strong as the muscles and tendons on the inside of the ankle.
Posterior tibial tendon – This tendon goes behind the ankle and around a bone inside the ankle (the medial malleolus) to help to maintain the arch of the foot along with other supportive ligaments.
Rheumatoid arthritis – An autoimmune disorder where the patient’s immune system malfunctions and attacks the cartilage and tendons.
Sprain – An injury causing tearing of a ligament, varying in severity. Injuries can range from a partial tearing of the ligament to a complete rupture.
Sprained ankle – A rupture of one or more of the ligaments of the ankle.
Talus – The ankle bone that sits within the ankle hinge made up of the two leg bones (tibia and fibula). Three joints are present. 1. The ankle joint allows the up and down motion of the foot with the leg. 2. The subtalar joint allows “inversion” and “eversion” of the foot with the leg. 3. The talonavicular joint that controls flexibility of the foot and the arch of the foot with a complicated biomechanical function. The talus is mostly covered with cartilage and has no muscular attachments making injuries difficult to heal.
Tendon – A structure in the body made mostly of collagen that connects muscle to bone. As the muscle contracts, it pulls on the tendon to move the bone. Tendons can tear or rupture if they are pulled too hard by the muscle, or if they have degenerated. Tendon inflammation is called tendonitis.
Tendonitis – Inflammation of a tendon usually caused by some injury, overuse or a mechanical abnormality in the foot or ankle. Treatment depends on the tendon, the extent of the inflammation and the length of time symptoms have been present.
Tendonosis – A later stage of tendonitis where the tendon starts to tear and fray.
Tibia (shinbone) – The large bone of the leg that extends from the ankle to the knee.
Tibialis anterior tendon – Moves the ankle upwards and stabilizes the foot in the latter part of the stance phase of gait. It extends the foot at the beginning and middle portions of the swing phase of gait.
Valgus – A tilt “outward” or away from the midline of the body.
Varus – A tilt “inward” or towards the midline of the body.
Areas of Focus
- Foot, Ankle & Lower Leg
- Achilles Tendinitis - Achilles Insertional Calcific Tendinopathy (ACIT)
- Achilles Tendon Rupture
- Achilles Tendonitis
- Ankle Fracture Surgery
- Ankle Fractures (Broken Ankle)
- Ankle Fusion Surgery
- Arthroscopic Articular Cartilage Repair
- Arthroscopy Of the Ankle
- Bunions
- Charcot Joint
- Common Foot Fractures in Athletes
- Foot Stress Fractures
- Hallux Rigidus Surgery - Cheilectomy
- Hammer Toe
- High Ankle Sprain (Syndesmosis Ligament Injury)
- Intraarticular Calcaneal Fracture
- Lisfranc Injuries
- Mallet, Hammer & Claw Toes
- Metatarsalgia
- Morton’s Neuroma
- Neuromas (Foot)
- Orthopedic Physician Or A Podiatrist? Definition of a Podiatrist
- Plantar Fasciitis
- Sports Foot Injuries
- Sprained Ankle
- Total Ankle Replacement
- Turf Toe
10 Questions To Ask Your Doctor About Total Ankle Replacement
Download our free questionnaire “10 Questions To Ask Your Doctor About Total Ankle Replacement.”

Andy McTear, Total Ankle Replacement Testimonial
MOVEWRIGHT™ Total Ankle Replacement
Patient Testimony Cassandra
Patient Testimony Dan
Patient Testimony Deven
Patient Testimony Jim
Patient Testimony Karen
Download The Patient Brochure for MOVERIGHT™ Total Ankle Replacement Brochure
Learn more about the INBONE® Total Ankle System by downloading the brochure.

The following Florida Orthopaedic Institute physicians specialize in Total Ankle Replacement:
Specialties
- AC Joint Injuries
- Achilles Tendinitis - Achilles Insertional Calcific Tendinopathy (ACIT)
- Achilles Tendon Rupture
- Achilles Tendonitis
- ACL Injuries
- Ankle Fracture Surgery
- Ankle Fractures (Broken Ankle)
- Ankle Fusion Surgery
- Anterior Cervical Corpectomy & Discectomy
- Arthroscopic Articular Cartilage Repair
- Arthroscopic Chondroplasty
- Arthroscopic Debridement of the Elbow
- Arthroscopy Of the Ankle
- Articular Cartilage Restoration
- Artificial Disk Replacement (ADR)
- Aspiration of the Olecranon Bursa - Fluid In Elbow
- Atraumatic Shoulder Instability
- Avascular Necrosis (Osteonecrosis)
- Bankart Repair
- Basal Joint Surgery
- Bicep Tendon Tear
- Bicep Tenodesis
- Bone Cement Injection
- Bone Growth Stimulation
- Bone Health Clinic
- Broken Collarbone
- Bunions
- Bursitis of the Shoulder (Subacromial Bursitis)
- Calcific Tendinitis of the Shoulder
- Carpal Tunnel Syndrome
- Charcot Joint
- Chiropractic
- Clavicle Fractures
- Colles’ Fractures (Broken Wrist)
- Common Foot Fractures in Athletes
- Community Outreach
- Cubital Tunnel Syndrome
- De Quervain's Tenosynovitis
- Deep Thigh Bruising
- Degenerative Disk Disease
- Diffuse Idiopathic Skeletal Hyperostosis (DISH)
- Discectomy
- Discitis Treatment & Information
- Dislocated Shoulder
- Dupuytren’s Disease
- Elbow
- Elbow Bursitis
- Elbow Injuries & Inner Elbow Pain in Throwing Athletes
- Epidural Injections for Spinal Pain
- Finger Dislocation
- Flexor Tendonitis
- Foot Stress Fractures
- Foot, Ankle & Lower Leg
- Foraminotomy
- Fractured Fingers
- Fractures Of The Shoulder Blade (Scapula)
- Fractures Of The Tibial Spine
- Functional Nerve Transfers of The Hand
- Ganglion Cysts
- General Orthopedics
- Glenoid Labrum Tear
- Golfer's Elbow
- Groin Strains and Pulls
- Growth Plate Injuries Of The Elbow
- Hallux Rigidus Surgery - Cheilectomy
- Hammer Toe
- Hamstring Injuries
- Hand & Finger Replantation
- Hand & Wrist
- Hand Nerve Decompression
- Hand Skin Grafts
- Hand, Wrist, Elbow & Shoulder
- Heat Injury/Heat Prostration
- High Ankle Sprain (Syndesmosis Ligament Injury)
- Hip & Thigh
- Hip Arthroscopy
- Hip Dislocation
- Hip Flexor Strains
- Hip Fractures
- Hip Hemiarthroplasty
- Hip Impingement Labral Tears
- Hip Muscle Strains
- Hip Pointers and Trochanteric Bursitis
- Hyperextension Injury of the Elbow
- Iliopsoas Tenotomy
- Iliotibial Band Syndrome
- Impingement Syndrome of the Shoulder
- Interlaminar Implants
- Interlaminar Lumbar Instrumental Fusion: ILIF
- Interventional Pain Management
- Interventional Spine
- Intraarticular Calcaneal Fracture
- Joint Replacement
- Knee & Leg
- Kyphoplasty (Balloon Vertebroplasty)
- Kyphosis
- Labral Tears Of The Hip (Acetabular Labrum Tears)
- Laminectomy: Decompression Surgery
- Lateral Collateral Ligament (LCL) Injuries
- Lisfranc Injuries
- Little League Shoulder
- LITTLE LEAGUER'S ELBOW (MEDIAL APOPHYSITIS)
- Lumbar Epidural Steroid Injection
- Lumbar Interbody Fusion (IBF)
- MACI
- Mallet, Hammer & Claw Toes
- Medial Collateral Ligament Injuries
- Meniscus Tears
- Metatarsalgia
- Minimally Invasive Spine Surgery
- Morton’s Neuroma
- Muscle Spasms
- Muscle Strains of The Calf
- Nerve Pain
- Neuromas (Foot)
- Neurosurgery
- Olecranon Stress Fractures
- Orthopaedic Total Wellness
- Orthopaedic Trauma
- Orthopedic Physician Or A Podiatrist? Definition of a Podiatrist
- Osteoarthritis of the Hip
- Osteoporosis
- Outpatient Spine Surgery
- Partial Knee Replacement
- Patellar Fracture
- Pelvic Ring Fractures
- Peripheral Nerve Surgery (Hand) Revision
- Pinched Nerve
- Piriformis Syndrome
- Piriformis Syndrome
- Plantar Fasciitis
- Plastic Surgery
- Podiatry
- Primary Care Sports Medicine
- Quadriceps Tendon Tear
- Radial Tunnel Syndrome (Entrapment of the Radial Nerve)
- Revascularization of the Hand
- Reverse Total Shoulder Replacement
- Rheumatoid Arthritis (RA) of the Shoulder
- Rheumatoid Arthritis Of The Hand
- Robotics
- Rotator Cuff Tears
- Runner's Knee
- Sacroiliac Joint Pain
- Sciatica
- Scoliosis
- Senior Strong
- Shin Splints
- Shoulder
- Shoulder Arthritis
- Shoulder Arthroscopy
- Shoulder Injury: Pain In The Overhead Athlete
- Shoulder Replacement
- Shoulder Separations
- Shoulder Socket Fracture (Glenoid Fracture)
- SLAP Tears & Repairs
- Spinal Fusion
- Spine
- Spondylolisthesis and Spondylolysis
- Sports Foot Injuries
- Sports Hernias (Athletic Pubalgia)
- Sports Medicine
- Sports Wrist and Hand Injuries
- Sprained Ankle
- Sprained Wrist Symptoms and Treatment
- Subacromial Decompression
- Sudden (Acute) Finger, Hand & Wrist Injuries
- Targeted Muscle Reinnervation (TMR)
- Tendon Transfers of The Hand
- Tennis Elbow Treatment
- Thigh Fractures
- Thigh Muscle Strains
- Thumb Ulnar Collateral Ligament Injuries
- Total Ankle Replacement
- Total Hip Arthroplasty
- Total Hip Replacement - Anterior Approach
- Total Knee Replacement Surgery
- Trapezius Strain (Muscle Strain of The Upper Back)
- Traumatic Shoulder Instability
- Tricep Pain & Tendonitis
- Trigger Finger
- Turf Toe
- UCL (Ulnar Collateral Ligament) Injuries
- Ulnar Neuritis
- Valgus Extension Overload
- Vertebroplasty
- WALANT (Wide Awake Local Anesthesia No Tourniquet)
- Whiplash and Whiplash Associated Disorder (WAD)
- Wound Care
- Wrist Arthroscopy
- Wrist Fractures
- Wrist Tendonitis
Services
- Physical Medicine & Rehabilitation
- Physical Therapy
- Primary Care Sports Medicine
- PROMs (Patient-Reported Outcome Measures)
- Same-Day Orthopaedic Appointments Now Available
- Sports Medicine
- Sports-Related Concussion Treatment
- Telehealth Page
- Telemedicine
- Workers' Compensation
- Workers' Compensation Dispensary
- X-Ray





