Multidirectional shoulder instability
Your shoulders enable you to carry out essential functions such as raising your arms, picking up objects, and lifting items with any weight. Unfortunately, these actions leave your shoulders vulnerable to various physical issues. One such concern is atraumatic shoulder instability.
Anatomy
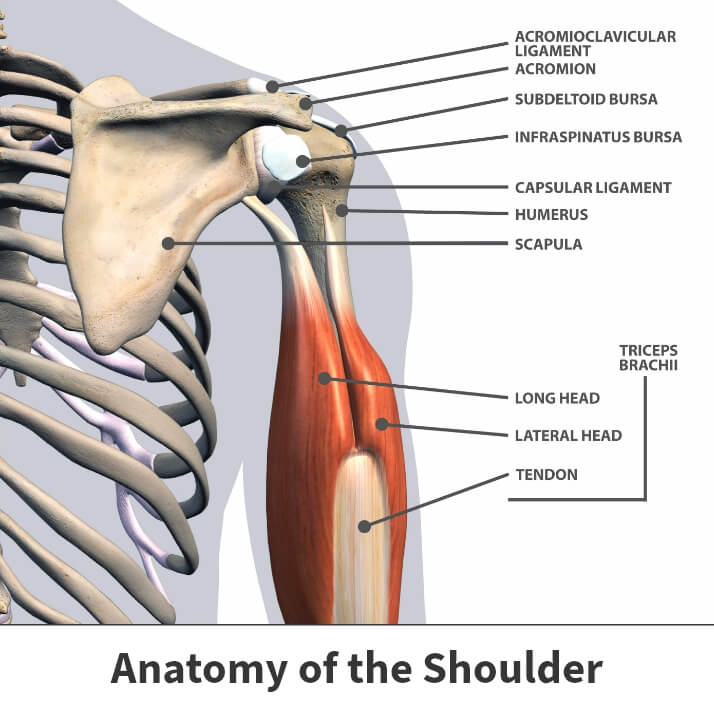
The shoulders are large ball and socket joints connecting the long bone of your upper arm bone (the humerus) to the shoulder blade (the scapula). In addition to the joint, your shoulders are made up of many vital soft tissues and muscles. Since the shoulder provides a great range of motion for athletic activities, it is also at a risk for dislocations.
About
Atraumatic shoulder instability occurs when the shoulder’s joint and other components slip apart due to reasons other than a traumatic event like a fall or automobile accident. These events are known medically as dislocations. In atraumatic shoulder instability, the head of the humerus can slowly, over time, slip out of its socket.
Causes
There are certain notable causes for atraumatic shoulder instability. The most common underlying factor is some type of existing but minor damage to a shoulder component that gradually worsens. Other possible explanations include muscle or soft tissue defects, unusually weak shoulder structures, or engaging in forceful or violent movements that place undue strain on the shoulder joint. Repetitive overhead motions (like those used for swimming), can overwork and stretch the muscles of the shoulder capsule, leading to chronic shoulder instability.
Risk factors
Certain contributing shoulder abnormalities can be genetic. You may stand at an increased risk provided a close family member developed the condition.
Additionally, athletes who frequently use their shoulders have a greater probability of sustaining atraumatic shoulder instability. Particularly at risk are those participating in:
- Golf
- Gymnastics
- Swimming
- Tennis
- Volleyball
Swimmers may be the most susceptible because of the continual overhead movements they make.
Types
Shoulder dislocations leading to instability are divided into three categories: anterior, posterior, and multi-directional.
- Anterior dislocations occur in the shoulder’s frontal region
- Posterior events happen in the shoulder’s rear
- Multi-directional dislocations can occur any direction

Symptoms
You might have some form of atraumatic shoulder instability if your shoulder often feels loose, unstable, and out of place. Varying degrees of discomfort can also go with the injury. The pain’s intensity will depend upon the dislocation’s location and severity. A serious case might significantly limit the mobility of your affected shoulder and arm. Recurring partial dislocations (subluxation) are another symptom.
Complications
If left untreated, major dislocations might lead to permanent shoulder deformity, chronic pain, and significant movement limitations.
Diagnosis
Your doctor will thoroughly examine your shoulder and have you perform specific tests designed to measure your shoulder’s motion range. Your physician may also investigate the shoulder joint’s stability.
If necessary, you might need to undergo a diagnostic imaging examination, such as magnetic resonance imaging (MRI), computerized tomography (CT scans), X-rays, or ultrasound. Each of these procedures captures internal photos of your shoulder and help confirm a diagnosis.
Treatment
The therapy chosen by your doctor will depend on the location and severity of the dislocation, its underlying cause, your age, your physical health, in addition to your athletic and fitness goals. Typically, many cases can be treated using nonsurgical efforts.
Nonsurgical treatments
Simple cases often resolve with rest. Moderate events are often treated with a course of physical therapy. This treatment is a tailored program of exercises created and overseen by a trained physical therapist. Physical therapy is designed to restrengthen the weakened shoulder joint and help it recapture lost motion ranges.
Surgical treatments
If rest and physical therapy are not successful or you are initially diagnosed with a serious dislocation, surgery may be needed. Typically, surgery centers on strengthening shoulder ligaments to improve general joint stability and prevent future dislocations.
Many of these operations are performed arthroscopically using a small, camera-equipped device called an arthroscope. These devices are less invasive and enable the surgeon to make the repairs without making larger shoulder incisions.
More complicated cases might need a larger incision in the shoulder’s front. Many of these operations are designed to fix the shoulder’s instability and are known as a capsular shift.
Recovery
It is difficult to offer an estimated recovery time. Every patient heals at their own pace. Moreover, several factors play an important part, including your:
- Age
- Health
- Injury type and severity
- Level of fitness
Another key factor is the type of treatment you received. If you had surgery, your recovery timetable will be longer than those who did not.
If you only used rest or physical therapy, the healing process could be completed in a matter of weeks. Recovery might take several to as many as six months if your shoulder was operated on.
Following surgery, your shoulder will need to be immobilized to allow for natural healing. Once the shoulder has healed sufficiently, you can begin a physical therapy program.
Following surgery, you should be able to return to normal physical activities. But you are strongly advised to engage in shoulder strengthening exercises ahead of such events. Dislocations tend to recur if you fail to keep your shoulder strong.
Videos
Related specialties
- AC Joint Injuries
- Bankart Repair
- Bicep Tenodesis
- Broken Collarbone
- Bursitis of the Shoulder (Subacromial Bursitis)
- Calcific Tendinitis of the Shoulder
- Clavicle Fractures
- Dislocated Shoulder
- Fractures of the Shoulder Blade (Scapula)
- Glenoid Labrum Tear
- Impingement Syndrome of the Shoulder
- Little League Shoulder
- Reverse Total Shoulder Replacement
- Rheumatoid Arthritis (RA) of the Shoulder
- Rotator Cuff Tears
- Shoulder Arthritis
- Shoulder Arthroscopy
- Shoulder Injury: Pain in the Overhead Athlete
- Shoulder Replacement
- Shoulder Separations
- Shoulder Socket Fracture (Glenoid Fracture)
- SLAP Tears & Repairs
- Subacromial Decompression
- Trapezius Strain (Muscle Strain Of The Upper Back)
- Traumatic Shoulder Instability
