Anterior shoulder dislocation reduction
Traumatic shoulder instability
Your shoulders support the weight of your upper body, extend your arms, and perform basic lifting and carrying motions. The pressure placed on them makes them susceptible to many different injuries. One such condition is traumatic shoulder instability.
Anatomy
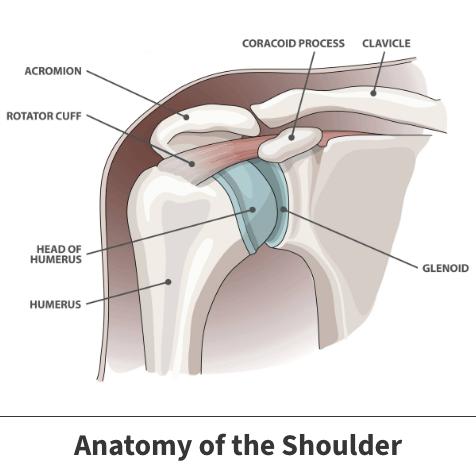
The shoulder is a complex structure. It is a ball and socket joint made up of separate parts, including:
- The primary shoulder joint, connecting the arm and shoulder bones
- Soft tissues, like ligaments and tendons, which connect larger structures like muscles and bones
- The rotator cuff, which is responsible for moving your shoulder
- The shoulder blade bone (the glenoid)
- The long arm bone (the humerus)
Many cases of traumatic shoulder instability are injuries to the cartilage protecting the shoulder joint and humerus (the labrum).
About
Anterior shoulder dislocation reduction, also known as traumatic shoulder instability, occurs when any part of the shoulder sustains some type of repetitive, chronic, or forceful contact that causes a weakened shoulder. These injuries could result from a severe and unexpected event that causes immediate and significant damage. The injury affects the injured shoulder’s ability to move freely and function properly.
One of the more common specific traumatic instability occurrences is ligament tears near the glenoid bone.
Another occurrence is a SLAP tear or lesion, with SLAP being an acronym for the Superior Labrum, Anterior And Posterior.
One other common form of traumatic shoulder instability is TUBS syndrome. TUBS is short for Traumatic Anterior Shoulder Instability. It is also referred to as a Bankart lesion.
Causes
Traumatic shoulder instability is often linked to full-contact sports, which exposes the shoulder to potential abuse and blunt force trauma. Specific high-risk sports include football, wrestling, and skiing. Non-sports injuries often result from spur-of-the-moment incidents, like falls, physical assaults, or car accidents.

Symptoms
In most cases, the primary symptom of traumatic shoulder instability is pain. Discomfort is often worsened when you move the shoulder and in forceful motions like throwing a ball or lifting and carrying objects. Visual clues, such as redness, bruising, and swelling, can also be present.
More serious incidents might include the feeling of instability, continual and debilitating discomfort, difficulty performing basic movements, and a gradual loss of motion. The most severe cases might prevent you from moving your shoulder at all.
Complications
If not diagnosed and treated early, traumatic shoulder instability will likely worsen. This could result in more severe pain and potentially serious problems like increased instability and life-limiting mobility issues.
Diagnosis
Confirmation of a traumatic shoulder instability-producing injury is usually performed in specific steps.
During the first step, your doctor will take your medical history, inquire about when the pain started, if you participated in any contact sports, or were recently involved in some type of fall or accident.
The next step typically involves a thorough examination of your shoulder. Your physician may ask you to perform specific movements to determine the structure’s motion range and strength. They may touch your shoulder at various points to identify areas of pain or tenderness.
In many instances, conclusions will need the use of diagnostic imaging equipment. Imaging equipment like X-rays, MRI (magnetic resonance imaging), and CT scans (computerized tomography) capture internal photos of your shoulder, which can reveal structural damage and other abnormalities.
Treatment
Traumatic shoulder instability is a significant physical injury. The specific treatment you will receive will hinge on factors such as your age, general health, the instability’s severity, the affected shoulder region, and fitness goals. For example, professional athletes may need more aggressive treatment to speed up their return to play.
Nonsurgical treatments
Mild to moderate cases can be treated using classic recovery measures like resting the injured shoulder and immobilizing it in a movement-restricting device like a sling or brace. Ice can also be applied to relieve discomfort and reduce associated swelling. Nonsurgical treatments might also be followed by a period of physical therapy geared towards preventing motion loss and weakening. Your Florida Orthopaedic Institute physician will guide you with a specific non-surgical treatment plan.
Surgical procedures
In cases where you experience noticeable shoulder instability or complete dislocation, surgery may be necessary. Several surgical procedures are performed to remove damaged components and correct dislocations by reattaching dislocated components.
Prognosis
Your recovery will depend on the severity of your injury and the specific treatment used to treat it. Specific recovery periods are difficult to estimate since everyone heals at their own pace.
Your recovery will take longer if you undergo surgery, as you will most likely need physical therapy.
Videos
Related specialties
- AC Joint Injuries
- Atraumatic Shoulder Instability
- Bankart Repair
- Bicep Tenodesis
- Broken Collarbone
- Bursitis of the Shoulder (Subacromial Bursitis)
- Calcific Tendinitis of the Shoulder
- Clavicle Fractures
- Dislocated Shoulder
- Fractures of the Shoulder Blade (Scapula)
- Glenoid Labrum Tear
- Impingement Syndrome of the Shoulder
- Little League Shoulder
- Reverse Total Shoulder Replacement
- Rheumatoid Arthritis (RA) of the Shoulder
- Rotator Cuff Tears
- Shoulder Arthritis
- Shoulder Arthroscopy
- Shoulder Injury: Pain in the Overhead Athlete
- Shoulder Replacement
- Shoulder Separations
- Shoulder Socket Fracture (Glenoid Fracture)
- SLAP Tears & Repairs
- Subacromial Decompression
- Trapezius Strain (Muscle Strain Of The Upper Back)