Epidural injections for spinal pain
Epidural injections are one of many methods doctors use to eliminate pain if a patient is not responding to conservative treatments such as physical therapy or oral medications. Epidural injections are when an anesthetic and an anti-inflammatory medication, such as cortisone (a steroid), is injected near the affected nerve, diminishing pain. Pain relief varies among patients. Multiple epidural injections may be required to eliminate pain completely.
Anatomy
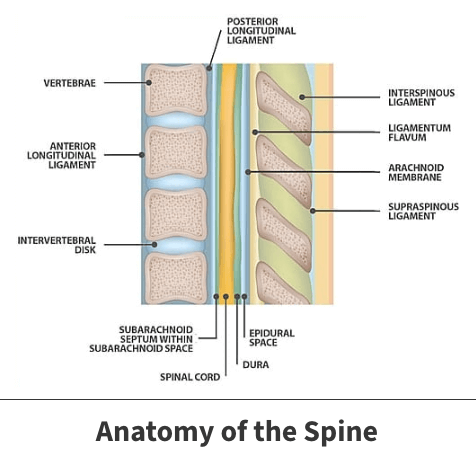
The spine consists of 33 individual bones (vertebrae) that interlock. The vertebrae are categorized into five regions:
- Cervical
- Thoracic
- Lumbar
- Sacrum
- Coccyx
An epidural injection is made in the epidural space located in the Lumbar region between the membrane surrounds the spinal cord (the dura mater) and the vertebral wall containing fat and small blood vessels. Other regions of the spine are also used for epidural injections. This space is located outside the dural sac which surrounds the nerve roots and is filled with cerebrospinal fluid.
About
Epidural injections use both an anesthetic and an anti-inflammatory medication, such as a steroid (cortisone) into a nerve in the spinal cord. They are used to treat pain that starts in the spine and radiates throughout the body due to a “pinched nerve” (a nerve that is inflamed or compressed). Epidural injections provide a temporary or prolonged relief from pain stemming from inflammation in the spine or extremities.
Many times the injection alone is enough to provide relief, but an epidural steroid injection is commonly used in combination with a comprehensive rehabilitation program to provide additional benefit. The rehabilitation program nearly always includes an exercise program to improve or maintain spinal mobility (stretching exercises), and stability (strengthening exercises).
An epidural injection may be used to reduce pain caused by:
- A herniated or bulging disc that impinges nerves causing pain
- Spinal stenosis
- Post-operative “failed back” surgery syndromes (chronic back or leg pain after spinal surgery)
- Bone spurs
- Other injuries to spinal nerves, vertebrae, and surrounding tissues

Diagnosis
In addition to treatment, epidural injections are also used for diagnosis. An epidural spinal injection can be done to a specific, isolated nerve to determine if that particular nerve is the source of the pain. The immediate reaction to the injection is monitored. If there is little pain relief, then that nerve is not the source of the pain. If the pain is completely or nearly relieved, then that nerve is the primary cause of pain. Once the nerve is located, it can then be treated. Your Florida Orthopaedic Institute physician will evaluate your symptoms and help determine the cause of your chronic pain.
Some people are not good candidates for spinal injections. These include people with:
- Skin infection at the site of needle puncture
- Bleeding disorder or anticoagulation
- Uncontrolled high blood pressure or diabetes
- Allergy to contrast, anesthetics, or steroids
Treatment
Epidural injections are performed under X-ray guidance, called fluoroscopy, which confirms safety and correct placement of the injection. A liquid contrast dye is injected first to ensure it will flow to the exact location. The needle is repositioned and more dye is injected until the proper flow is achieved. The epidural is then injected, delivering steroids directly to the epidural space. Sometimes extra fluids (local anesthetic and/or a normal saline solution), are used to help flush out inflammatory objects from around the area that may be contributing to the source of pain.
Post procedure
The results after receiving an epidural injection depend on the initial cause of the patient’s pain. It may take up to two to three days until pain relief occurs. If there is immediate discomfort, an ice pack can be placed on the affected area. The pain relief varies from person to person but may last up to one year after the initial procedure. Depending on the pain relief after the initial procedure, the patient may not need additional epidural injections. But if the pain reoccurs then additional epidural injections may be necessary. To help with strength and mobility, a combination of rehabilitative exercise and physical therapy may be prescribed to help minimize the future existence of pain in the affected area. Your Florida Orthopaedic Institute physician will help determine the best post-procedure plan for you.
Videos
Related specialties
- Anterior Cervical Corpectomy & Discectomy
- Artificial Disc Replacement (ADR)
- Bone Cement Injection
- Degenerative Disc Disease
- Diffuse Idiopathic Skeletal Hyperostosis (DISH)
- Discectomy
- Discitis Treatment & Information
- Foraminotomy
- Interlaminar Implants
- Interlaminar Lumbar Instrumental Fusion: ILIF
- Kyphoplasty (Balloon Vertebroplasty)
- Kyphosis
- Laminectomy: Decompression Surgery
- Lumbar Epidural Steroid Injection
- Lumbar Interbody Fusion (IBF)
- Minimally Invasive Spine Surgery
- Outpatient Spine Surgery
- Pinched Nerve
- Piriformis Syndrome
- Sacroiliac Joint Pain
- Sciatica
- Scoliosis
- Spinal Fusion
- Spondylolisthesis & Spondylolysis
- Vertebroplasty
- Whiplash & Whiplash Associated Disorder (WAD)
