Whiplash & whiplash associated disorder (WAD)
Whiplash and whiplash associated disorders (WAD) occur when the neck suffers a rapid forward or backward movement. They can have varying symptoms—anywhere from mild to severe. Whiplash is treated in many different ways, but in most cases, it is treated non-surgically with physical therapy, exercises and medication. If symptoms are severe, then surgery may be recommended.
Anatomy
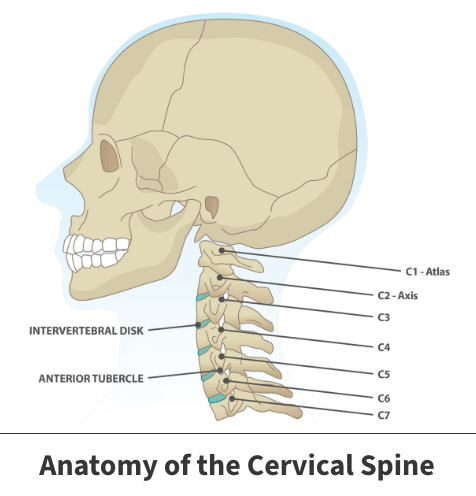
The spine consists of 33 individual bones (vertebrae) that interlock. The vertebrae are categorized into five regions:
- Cervical
- Thoracic
- Lumbar
- Sacrum
- Coccyx
The cervical region of the spine supports the head, protects the nerves and spinal cord and allows for the neck to move.
Intervertebral discs sit between the vertebrae and are the shock absorbers for the spine. They are flat, round, about half an inch thick and made of two components—the nucleus pulposus, and the annulus fibrosus. The nucleus has a jelly-like consistency and is found in the center of the disc. The “jelly” allows the disc to be flexible and strong. The annulus is the flexible outer ring of the disc and consists of several layers. When moving or standing, weight is put on the nucleus, causing it to expand while the annulus holds it in place. Together, the nucleus and annulus allow for movement to take place while simultaneously maintaining the strength of the spine. Many nerve endings supply the annulus and, as a result, an injured annulus can cause pain.
About
Whiplash is a common injury that is often mistreated or ignored due to a lack of understanding of the condition. When you quickly accelerate or decelerate, the force of that movement causes unrestrained, rapid forward and backward movement of your head and neck. That neck and head movement is whiplash. For example, during a car accident, the abrupt stop caused by the crash causes your head and neck to move rapidly, resulting in whiplash. Whiplash can damage both the bone structures and soft tissues in the neck. In more severe cases, it can cause whiplash associated disorders (WAD). On average, approximately 30% to 50% of patients who sustain a whiplash injury are going to report chronic and potentially more widespread symptoms, also known as WAD.
Symptoms
Symptoms associated with whiplash include:
- Neck pain and stiffness
- Shoulder pain and stiffness
- Headache
- Dizziness
- Fatigue
- Jaw pain
- Back pain
- Arm pain and weakness
- Visual disturbances
- Ringing in the ears
In more severe and chronic cases of whiplash associated disorder, the following symptoms may be present:
- Depression
- Frustration
- Anger
- Anxiety
- Stress
- Post-traumatic stress disorder
- Drug dependency
- Sleep disturbances, such as insomnia

Diagnosis
Your Florida Orthopaedic Institute physician will look at your symptoms to make sure that there is no significant injury to the neck, head, or rest of the body that would need immediate treatment. They will ask about how you sustained the injury and perform a physical exam. After, your physician will decide which tests, if any, will be needed to determine how severe the injury is. These tests can include:
- X-rays – X-rays may be taken to see if any bones were broken or if the spine is not stable. X-ray images will also show the disc height and bone spurs.
- EMG/NCV (electromyography and nerve conduction velocity) – This test may be used if your physician suspects that a nerve is trapped or if nerve damage is present.
- Discography – Discography is a disc injection that shows if a disc is contributing to the pain. This test is only used for patients with severe pain that has not improved despite being treated.
- MRI (magnetic resonance imaging) scan – MRI scans are used if your physician thinks you may have disc herniation, disc injury or compression of a nerve in the spinal cord.
- CT (computed tomography) scan – CT scans are used to help diagnose neck pain that does not respond to treatment.
Treatment
The goals of whiplash treatment are to control pain, restore normal range of motion in your back and neck, so you can return to your normal activities. Your specific treatment plan will depend on the severity of your whiplash injury or whiplash associated disorder. Most cases are treated nonsurgically. In rare cases, surgery may be required.
Nonsurgical treatments
Many nonsurgical treatments can help reduce and eliminate your symptoms. To help with pain, your physician may recommend one or more of the following treatments:
- Rest –This is most useful during the first 24 hours after receiving the injury. However, too much rest may actually delay your recovery.
- Heat or cold – Applying heat and cold to the neck can help reduce pain.
- Pain medications – Over-the-counter pain relievers such as Tylenol (acetaminophen) and Advil/Motrin (ibuprofen) can control mild to moderate whiplash pain.
- Prescription medications – If your pain is more severe, stronger prescription pain relievers can help diminish pain.
- Injections – Injections such as lidocaine, a numbing medicine, applied to painful muscle areas can also help decrease pain.
- Muscle relaxants – These help to loosen tight muscles that may be causing pain.
Exercise (specifically stretching movement exercises) may be recommended to help restore your range of motion in your neck, allowing you to resume your normal activities. These exercises may involve rotating your neck in both directions, tilting your head side to side, rolling your shoulders, and bending your neck toward your chest.
Your physician may also recommend physical therapy if you have ongoing whiplash pain or need help with range of motion exercises. Your physician will help determine the best physical therapy option for you.
Learn More About Physical Therapy
In some cases, foam collars are recommended to help hold the neck still, allowing it to heal. Your physician will decide exactly how long you should wear the foam collar to promote healing and prevent further injury.
Surgical treatments
If your condition hasn’t improved after extensive nonsurgical treatment, an operation may be your best option. In cases of a ruptured or herniated disc located in the spine, your surgeon may decide to remove all parts of the damaged disc in a process called a discectomy. During this procedure, your surgeon stabilizes the spine using one of the following procedures:
- Artificial disc replacement (ADR) – An artificial disc is implanted where the injured disc was removed. This procedure preserves and restores neck movement.
- Spinal fusion – If the disc is not removed, spinal fusion may be performed on the spine. Bones in the spine are fused together so that they heal into a single, solid bone, stabilizing the spine.
If the whiplash caused any damage to the spinal cord or nerves, then one of the following procedures may be performed:
- Corpectomy – This procedure involves removing part of the vertebrae to reduce pressure on the spinal cord and nerves if that is the source of the pain.
- Laminectomy or laminoplasty – Both of these procedures focus on the lamina, the bony plate that’s at the back of each vertebra (The lamina protects your spinal cord and spinal canal). If the lamina is pressing on your spinal cord, the surgeon makes more room for the cord by performing a laminectomy (removing all or part of the lamina) or a laminoplasty (reshaping the lamina to create more room for your spinal cord).
- Foraminotomy – If there is a narrowing of the space where the nerve exits the spinal canal, a foraminotomy may be performed which removes the foramen (the area where the nerve roots exit the spinal canal). This procedure increases the size of the nerve pathway, making it less likely that the nerve will be pinched or compressed.
Your Florida Orthopaedic Institute physician will help chose the best procedure for you.
Videos
Related specialties
- Anterior Cervical Corpectomy & Discectomy
- Artificial Disc Replacement (ADR)
- Bone Cement Injection
- Degenerative Disc Disease
- Diffuse Idiopathic Skeletal Hyperostosis (DISH)
- Discectomy
- Discitis Treatment & Information
- Epidural Injections for Spinal Pain
- Foraminotomy
- Interlaminar Implants
- Interlaminar Lumbar Instrumental Fusion: ILIF
- Kyphoplasty (Balloon Vertebroplasty)
- Kyphosis
- Laminectomy: Decompression Surgery
- Lumbar Epidural Steroid Injection
- Lumbar Interbody Fusion (IBF)
- Minimally Invasive Spine Surgery
- Outpatient Spine Surgery
- Pinched Nerve
- Piriformis Syndrome
- Sacroiliac Joint Pain
- Sciatica
- Scoliosis
- Spinal Fusion
- Spondylolisthesis & Spondylolysis
- Vertebroplasty