Research & academics
Advancing orthopedics through our research & academics
FOI physicians and those we train adopt the latest advancements and techniques in orthopedics. Our commitment to new research and technological advancements ensures that patients receive the highest quality of care.
Foundation for Orthopaedic Research & Education (FORE)
FORE is a non-profit organization that was founded in 1999 by surgeons at Florida Orthopaedic Institute with the mission to improve orthopedic medicine through research, innovation and education. FORE advances orthopedic excellence by focusing on clinical and biomechanical research, surgical training and continuing medical education (CME).
FORE’s clinical research department conducts orthopedic clinical trials in the following subspecialties: hand, foot, ankle, knee, hip, spine, elbow, shoulder, and sports medicine.
FORE partners with industry, research and educational foundations and orthopedic associations to
develop and evaluate promising biomechanical orthopedic technologies.
As an ACGME accredited provider of continuing medical education for patients, FORE facilitates the highest quality of patient care through education that enhances knowledge, skills and surgical technique.
Florida InnoVation & Education (FIVE) Labs
FIVE Labs is a state-of-the-art facility for biomechanical and clinical research. This 15,500-sq-ft. facility is centrally located only two miles from Tampa International Airport and less than five miles from Tampa General Hospital. FIVE Labs is part of US Bioskills, one of the largest bioskills networks in the country.
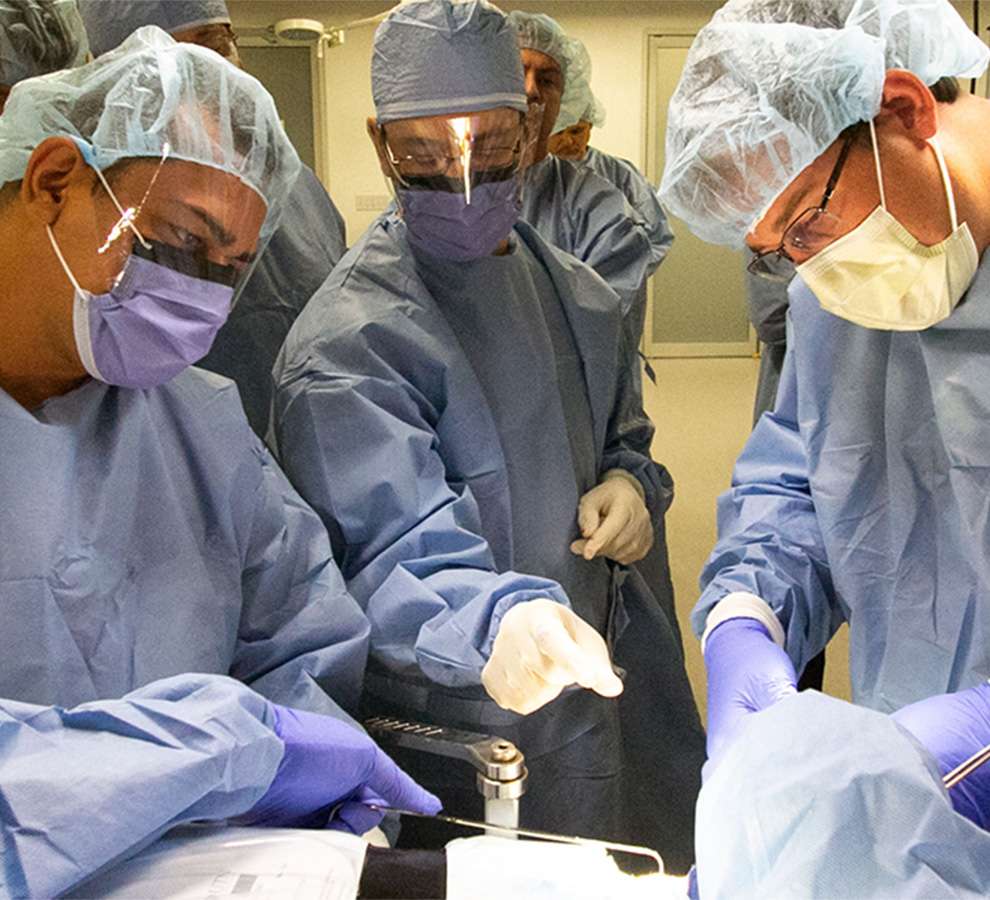
The Bioskills Lab has over 3,600 sq. ft. of customizable lab space suitable for small and large events. The lab is fully equipped for up to 30 surgical stations with monitors and cameras throughout. Live feed videos can be displayed throughout the facility or streamed over the web, allowing viewers to watch live events. The experienced team at FIVE Labs offers concierge level service to ensure successful events.
The Prototype Lab is designed to function as a 1 – 2 station bioskills lab and innovation hub. The Prototype Lab has direct access to the boardroom to increase engineering, design review and product development efficiency. The Prototype Lab features two surgical stations, HD video/audio recording and a floor-to-ceiling dry-erase wall to aid and capture the creative process.
The FIVE Labs Conference Center can accommodate large multi-day conferences, demonstration sessions for individual surgeons, sales training events or team brainstorming meetings. The in-house team of CME Coordinators/Event Planners provides accreditation, education, and conference management services for over 40 courses annually.
Engineers at FIVE Labs work side by side with surgeons and medical device professionals to develop new and innovative medical ideas. They have the experience to take these ideas from concept to prototype to final product. The studio offers rapid 3D CAD models and drawings, provisional and full utility patenting, and initial FDA documentation.
OTS Research
The Orthopaedic Trauma Service has a robust research program staffed with dedicated and experienced research nurse coordinators, statistician, and biomechanical engineers. Research staff assist OTS surgeons and fellows with all research tasks, including literature searches; protocol development; budget preparation; IRB submissions and coordination; preparation of grant applications; medical record and radiograph collection for review; consenting research subjects; scheduling of research studies (radiographic or laboratory studies); data collection, including completion of patient outcome measurement; photo and/or video documentation; data entry, validation and formatting; and documentation of IRBs and study sponsors. In addition, numerous USF and visiting orthopaedic residents and medical students participate in ongoing projects.
An OTS trauma registry is coordinated by a research coordinator. Admission variables are documented for patients who consent to be included in the registry, including fracture pattern, mechanism of injury, comorbidities, and injury and treatment variables. The registry is utilized to track the volume and type of fracture patterns treated, and to identify potential subjects for specific research projects.
The Journal of Orthopaedic Trauma (JOT) is devoted exclusively to the diagnosis and management of hard and soft tissue trauma, including injuries to bone, muscle, ligament, and tendons, as well as spinal cord injuries. The editor-in-chief and managing editor have their offices in Tampa.